What is Urinary Tract Infection (UTI)?
A urinary tract infection (UTI) refers to an infection that affects a part of the urinary tract, which includes the kidneys, ureters, urinary bladder, and urethra. Here are some important points about UTIs:
- Types of UTIs: UTIs can occur in different parts of the urinary tract. The most common type is bladder infection or cystitis, which affects the bladder. Infections can also occur in other areas, such as the kidneys (pyelonephritis), ureters, and urethra.
- Bacteriuria: Bacteriuria refers to the presence of bacteria in the urine. It is considered significant when there are 105 or more organisms per milliliter (108/1) in pure culture.
- Symptoms of Cystitis: Cystitis typically presents with symptoms such as frequent urination, pain or discomfort during urination (dysuria), suprapubic pain, and often the presence of pus in the urine (pyuria). Hematuria, which is blood in the urine, may also occur in some cases.
- Acute Urethral Syndrome: Acute urethral syndrome is a term used to describe the symptoms of acute cystitis accompanied by pyuria, even when no bacteria are detected by routine urine culture.
- Pyelonephritis: Pyelonephritis refers to an infection of the kidneys. It can cause symptoms such as loin pain (pain in the lower back or side), pyuria, chills (rigors), fever, and sometimes bacteria in the bloodstream (bacteremia).
- Etiology of UTIs: Most UTIs are caused by uropathogenic organisms that colonize the periurethral mucosa. These organisms typically originate from the gastrointestinal or vaginal flora and can ascend through the urethra to the bladder and other parts of the urinary tract.
- Common Pathogens: The most common pathogens associated with UTIs include Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis, and Staphylococcus saprophyticus. However, the specific causative organism can vary depending on the individual and other factors.
- Global Prevalence: UTIs are a significant public health problem worldwide, affecting approximately 150 million people each year. The high prevalence emphasizes the importance of proper diagnosis, treatment, and prevention of UTIs.
UTIs can cause discomfort and may lead to complications if left untreated. Prompt medical attention, appropriate antimicrobial therapy, and preventive measures, such as good hygiene and proper fluid intake, are crucial for managing and preventing UTIs.
Types of Urinary Tract Infection (UTI)
Urinary tract infections (UTIs) can affect different parts of the urinary tract, leading to varying symptoms. Here are the types of UTIs and their associated signs and symptoms:
- Kidney Infection (Pyelonephritis): When the infection reaches the kidneys, it is known as pyelonephritis. Signs and symptoms of a kidney infection may include:
- Back or side pain (usually below the ribs)
- High fever
- Shaking and chills
- Nausea and vomiting
- Bladder Infection (Cystitis): Bladder infections are the most common type of UTIs. Symptoms of cystitis may include:
- Pelvic pressure
- Lower belly discomfort or pain
- Frequent urge to urinate
- Pain or burning sensation during urination (dysuria)
- Blood in the urine (hematuria)
- Urethral Infection (Urethritis): Urethritis refers to an infection of the urethra, the tube through which urine exits the body. Symptoms of urethritis can include:
- Burning or pain during urination (dysuria)
- Discharge from the urethra
It’s important to note that these symptoms can vary from person to person, and some individuals may experience a combination of symptoms from different types of UTIs. Additionally, certain conditions or complications can result in a more severe presentation of symptoms.
Causative Agents of UTI
Urinary tract infections (UTIs) can be caused by various bacteria and fungi. Here is some information about the causative agents of UTIs:
- Escherichia coli (E. coli): Uropathogenic Escherichia coli (UPEC) is the most common causative agent of both uncomplicated and complicated UTIs. It is a Gram-negative bacterium commonly found in the gastrointestinal tract and can enter the urinary tract, leading to infection.
- Other Bacteria in Uncomplicated UTIs: Following UPEC, other bacteria commonly associated with uncomplicated UTIs include:
- Klebsiella pneumoniae
- Staphylococcus saprophyticus
- Enterococcus faecalis
- Group B Streptococcus (GBS)
- Proteus mirabilis
- Pseudomonas aeruginosa
- Staphylococcus aureus
- Causative Agents in Complicated UTIs: In complicated UTIs, the prevalence of causative agents follows a similar pattern to uncomplicated UTIs, with UPEC being the most common. Other organisms commonly associated with complicated UTIs include:
- Enterococcus species
- Klebsiella pneumoniae
- Candida species (fungi)
- Staphylococcus aureus
- Proteus mirabilis
- Pseudomonas aeruginosa
- Group B Streptococcus (GBS)
- Concentration of Organisms: UTIs are typically caused by a single organism present in a high concentration, usually equal to or greater than 10^5 colony-forming units per milliliter (CFU/ml). This high concentration is indicative of an infection rather than contamination.
- Polymicrobial Infections: While UTIs are primarily caused by a single organism, polymicrobial infections (involving more than one microorganism) can occur in patients with anatomical abnormalities or foreign bodies in the urinary tract. However, the presence of multiple species in a culture may also indicate colonization or culture contamination, and careful consideration is needed to differentiate true infection from other causes.
Understanding the causative agents of UTIs is important for appropriate diagnosis and targeted treatment. It allows healthcare professionals to select appropriate antibiotics and manage infections effectively.
Risk factors of UTI
Several factors can increase the risk of developing a urinary tract infection (UTI). Here are some key risk factors associated with UTIs:
- Gender: UTIs are more common in females compared to males. This is because females have shorter urethras, which makes it easier for bacteria to enter the urinary tract from the nearby rectal area.
- Previous UTI: Having had a UTI in the past increases the risk of developing another infection.
- Sexual Activity: Sexual intercourse can introduce bacteria into the urethra, increasing the risk of UTIs. This risk is particularly high in women.
- Changes in Vaginal Flora: Alterations in the bacteria that naturally inhabit the vagina, known as vaginal flora, can make individuals more susceptible to UTIs. Factors such as menopause, use of spermicides, or certain hormonal changes can disrupt the balance of vaginal bacteria.
- Pregnancy: Pregnant women are more prone to UTIs due to hormonal changes and the pressure exerted on the urinary tract by the growing uterus.
- Age: UTIs are more common in certain age groups. Older adults and young children have an increased risk due to factors like weakened immune systems or difficulty with proper hygiene practices.
- Structural Abnormalities: Structural problems in the urinary tract, such as an enlarged prostate in males, can impede the normal flow of urine and contribute to UTIs.
- Poor Hygiene: Inadequate hygiene practices, especially in children who are potty-training, can facilitate the entry of bacteria into the urinary tract.
Symptoms of UTI
Urinary tract infections (UTIs) can present with different symptoms depending on the area of the urinary tract affected. Here are the common symptoms associated with UTIs:
Bladder Infection Symptoms:
- Pain or burning sensation during urination (dysuria)
- Frequent urination
- Urgency to urinate, even when the bladder is not full
- Hematuria (blood in the urine)
- Pressure or cramping in the groin or lower abdomen
Kidney Infection Symptoms:
- Fever
- Chills
- Lower back pain or pain in the side of the back
- Nausea or vomiting
It’s important to note that younger children may have difficulty expressing their symptoms. However, fever is the most common sign of UTIs in infants and toddlers. It’s worth mentioning that most children with fever do not have a UTI, so it’s crucial to consult a healthcare professional if you suspect a UTI in your child.
Pathogenesis of UTI
The pathogenesis of urinary tract infections (UTIs) involves the entry of bacteria into the urinary tract, attachment to the bladder wall, and subsequent infection. Here are some key points regarding the pathogenesis of UTIs:
- Entry of Bacteria: The most common route of entry for bacteria into the urinary tract is through the urethra. However, bacteria can also enter the urinary tract through the bloodstream or lymphatic system. It is believed that the bacteria responsible for UTIs are often transmitted from the bowel, with females being at higher risk due to their anatomical proximity of the urethra to the anus.
- Attachment to the Bladder Wall: Once the bacteria reach the bladder, they have the ability to attach to the bladder wall. The attachment is facilitated by specific mechanisms and adhesive structures on the bacterial surface. This attachment allows the bacteria to resist being flushed out during urination.
- Biofilm Formation: After attachment, many UTI-causing bacteria have the ability to form a biofilm on the bladder wall. A biofilm is a complex structure consisting of bacteria embedded in a matrix of substances, such as polysaccharides and proteins. The biofilm protects the bacteria from the host immune response and makes them more resistant to antibiotics, making it challenging to eliminate the infection.
- Infection and Symptoms: The presence of bacteria in the bladder and the formation of a biofilm lead to an inflammatory response by the body’s immune system. This immune response causes localized inflammation and can result in symptoms such as pain, frequent urination, and urinary discomfort. If left untreated, the infection can potentially spread to the kidneys, leading to more severe symptoms and complications.
Diagnosis of UTI
The diagnosis of urinary tract infections (UTIs) involves evaluating the patient’s symptoms and performing specific diagnostic tests. Here is some information about the diagnosis of UTIs:
- Uncomplicated UTI Diagnosis: In cases of uncomplicated UTIs, a reliable diagnosis can often be made based on typical symptoms alone. Urinalysis and urine culture are not routinely needed, and patients may be treated empirically without further testing.
- Diagnostic Tests for Complicated UTI: For suspected complicated UTIs, or when symptoms of pyelonephritis (kidney infection) are present, diagnostic tests including urinalysis and urine culture should be performed.
- Urinalysis: Urinalysis can be done using a dipstick or microscopic examination of the urine sample. Positive results for leukocyte esterase and nitrite reactions on the dipstick indicate the presence of infection. Most patients with UTI have pyuria (white blood cells in the urine), and proteinuria and hematuria (presence of blood in the urine) are also common findings.
- Gram Stain: Gram staining of urine samples may be useful in detecting significant bacterial growth. However, its sensitivity is limited and it is not recommended for routine use in urine specimens.
- Routine Culture: Routine urine culture involves inoculating a urine sample onto agar plates to quantitatively assess bacterial growth. The lower level of detection is typically 10^3 colony-forming units per milliliter (cfu/mL). The extent of further testing, such as identification and susceptibility testing, depends on factors such as the type of specimen, the number of species isolated, and the pathogenic potential of the isolates.
- Culture for Possible Complicated UTI: For patients at risk of complicated UTI, such as those with symptoms and lower bacterial quantities (<10^3-10^4 cfu/mL), culture methods using a 10-microliter inoculum can detect significant infections. The extent of workup follows similar guidelines used for routine cultures.
- Other Laboratory Testing: Additional laboratory testing may be appropriate depending on the clinical presentation. Pregnancy testing may be recommended for women with uncomplicated UTI. Blood cultures are advised for patients with complicated UTI who exhibit signs of systemic infection (e.g., fever, hypotension, or signs of sepsis).
Treatment of UTI
The primary approach to treating urinary tract infections (UTIs) involves the use of antibiotics. Here is some information about the treatment of UTIs:
- Uncomplicated and Complicated UTIs: For uncomplicated UTIs, the first-line treatment is typically oral trimethoprim. If trimethoprim is contraindicated or not suitable, oral nitrofurantoin can be used as a second-line option. In pregnancy, oral cephalexin is often prescribed.
- Pyelonephritis (Kidney Infection): Pyelonephritis, which is a more severe form of UTI involving the kidneys, usually requires intravenous (IV) antibiotics. The first-line treatment is IV co-amoxiclav (a combination of amoxicillin and clavulanic acid) along with IV gentamicin. If the first-line treatment is not suitable, oral or IV ciprofloxacin in combination with IV gentamicin can be used as a second-line option. In pregnancy, IV cefuroxime is often administered.
- Urethral Syndrome: Urethral syndrome, which is characterized by symptoms of dysuria and pyuria but without the presence of bacteria, does not respond well to antibiotics. The primary treatment approach for urethral syndrome is to increase fluid intake to flush out bacteria from the urethra.
- Complicated UTIs: Complicated UTIs are more challenging to treat and often require a more aggressive evaluation, treatment, and follow-up. The underlying complication contributing to the UTI needs to be identified and addressed along with appropriate antibiotic therapy.
- Concerns of Antibiotic Resistance: Increasing antibiotic resistance is a significant concern in the treatment of complicated and recurrent UTIs. It is important to monitor and address antibiotic resistance patterns to ensure effective treatment options are available in the future.
Treatment of Urinary Tract Infections with D-Mannose
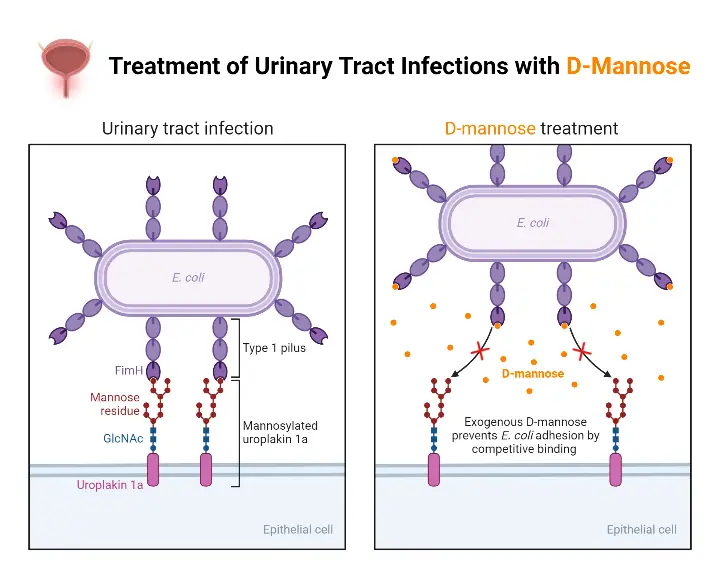
D-Mannose is a type of sugar that is commonly used as a natural remedy for urinary tract infections (UTIs). It is believed to work by preventing bacteria from attaching to the walls of the urinary tract and flushing them out of the body. Here’s some information about the treatment of UTIs with D-Mannose:
- Mechanism of action: UTIs are primarily caused by the colonization of bacteria, typically Escherichia coli (E. coli), in the urinary tract. D-Mannose is a simple sugar that is not metabolized by the body and is excreted through the urinary system. It is thought that D-Mannose attaches to the E. coli bacteria, preventing them from binding to the urinary tract walls, allowing them to be flushed out during urination.
- Effectiveness: D-Mannose has gained popularity as a natural remedy for UTIs, and some people report positive results. However, the scientific evidence supporting its effectiveness is limited. There have been a few small-scale studies and anecdotal reports suggesting that D-Mannose may help prevent or treat UTIs. Further research is needed to establish its true efficacy.
- Usage: D-Mannose is available as a supplement in the form of powder or capsules. The typical recommended dosage for treating UTIs is 1 to 2 grams of D-Mannose taken every few hours, followed by a maintenance dose of 0.5 to 1 gram taken once or twice daily. It is essential to follow the instructions provided by the manufacturer or consult with a healthcare professional for proper dosage and usage.
- Safety: D-Mannose is generally considered safe with minimal side effects. It is well-tolerated by most individuals, and there are no known drug interactions. However, it is a sugar, so people with diabetes should be cautious and monitor their blood sugar levels when using D-Mannose. As with any supplement or medication, it is recommended to consult with a healthcare professional before starting D-Mannose, especially if you have any pre-existing medical conditions or are taking other medications.
- Limitations: D-Mannose may be more effective in preventing UTIs rather than treating active infections. It is not considered a substitute for conventional antibiotic treatment in severe or recurrent UTIs. If you suspect you have a UTI, it is essential to seek medical attention for diagnosis and appropriate treatment. Your healthcare provider can determine the most suitable course of action based on your individual circumstances.
In summary, while D-Mannose is widely used as a natural remedy for UTIs, the scientific evidence supporting its efficacy is limited. It may be worth considering as a preventive measure or as a complementary approach alongside conventional treatments. However, it is crucial to consult with a healthcare professional for an accurate diagnosis and appropriate treatment plan.
Animation Video
Prophylaxis and Prevention of UTI
Prophylaxis and prevention strategies are important in reducing the risk of urinary tract infections (UTIs). Here is some information on UTI prophylaxis and prevention:
- Prophylactic Antibiotics: In children with recurrent UTIs, prophylactic antibiotics may be prescribed to prevent further infections and protect renal function. The use of prophylactic antibiotics should be guided by a healthcare professional.
- Hydration: Staying well hydrated is crucial in preventing UTIs. Drinking plenty of fluids, especially water, helps dilute urine and promotes frequent urination. This helps flush out bacteria from the urinary tract before an infection can develop.
- Urination After Sexual Activity: Emptying the bladder soon after sexual activity can help flush out bacteria that may have entered the urethra during intercourse. Additionally, drinking a full glass of water after sexual activity can further assist in flushing out bacteria.
- Personal Hygiene: Practicing good personal hygiene can reduce the risk of UTIs. Here are some recommendations:
- Wipe from front to back after urinating and after a bowel movement to prevent the spread of bacteria from the anus to the urethra and vagina.
- Minimize the use of potentially irritating feminine products such as deodorant sprays, douches, and powders, as they can irritate the urethra.
- Showering Instead of Bathing: Taking showers instead of baths can help reduce the risk of UTIs. Baths can increase the likelihood of bacteria entering the urethra, while showers promote better hygiene and reduce the chance of bacterial contamination.
- Consider Cranberry Juice: While the evidence on cranberry juice preventing UTIs is not conclusive, it is generally considered safe to consume and may have some benefit. Drinking cranberry juice may help inhibit bacterial adherence to the urinary tract, potentially reducing the risk of infection.
- Birth Control Methods: Certain birth control methods, such as diaphragms, unlubricated condoms, or condoms treated with spermicide, can contribute to bacterial growth. If recurrent UTIs are an issue, discussing alternative birth control options with a healthcare professional may be beneficial.
FAQ
What is a urinary tract infection (UTI)?
A urinary tract infection is an infection that affects any part of the urinary system, including the kidneys, bladder, ureters, and urethra.
Can UTIs be prevented?
While UTIs cannot always be prevented, there are steps you can take to reduce the risk. These include staying hydrated, urinating after sexual activity, practicing good hygiene, avoiding irritating products in the genital area, and considering cranberry juice or supplements.
Who is at a higher risk of developing UTIs?
Women are more prone to UTIs due to their shorter urethra, which allows bacteria to reach the bladder more easily. Other risk factors include sexual activity, menopause, urinary tract abnormalities, catheter use, weakened immune system, and certain medical conditions.
How are UTIs diagnosed?
UTIs are typically diagnosed based on symptoms, a physical examination, and a urine sample analysis. Urinalysis and urine culture may be conducted to confirm the presence of bacteria and determine the specific type of bacteria causing the infection.
What is the treatment for a UTI?
The mainstay of UTI treatment is antibiotics prescribed by a healthcare professional. The specific antibiotic and duration of treatment depend on the type and severity of the infection. It is important to complete the full course of antibiotics as prescribed.
Can UTIs be recurrent?
Yes, UTIs can recur, especially in individuals with risk factors such as urinary tract abnormalities, frequent sexual activity, or a history of UTIs. Recurrent UTIs may require further evaluation and management by a healthcare professional.
Are there any complications associated with UTIs?
If left untreated or inadequately treated, UTIs can potentially lead to more serious complications, such as kidney infections (pyelonephritis), bloodstream infections (sepsis), and recurrent infections.
What are the common symptoms of a UTI?
Common symptoms of a UTI may include frequent urination, pain or burning sensation during urination, cloudy or bloody urine, strong-smelling urine, pelvic pain, and a feeling of urgency to urinate.
Can men get UTIs?
Although less common, men can also develop UTIs. In men, UTIs are often associated with underlying urinary tract abnormalities, such as an enlarged prostate or urinary stone.
When should I seek medical attention for a suspected UTI?
If you experience symptoms of a UTI, it is recommended to seek medical attention. Prompt diagnosis and treatment can help alleviate symptoms and prevent potential complications.
References
- https://www.mayoclinic.org/diseases-conditions/urinary-tract-infection/symptoms-causes/syc-20353447
- https://www.cdc.gov/antibiotic-use/uti.html
- https://my.clevelandclinic.org/health/diseases/9135-urinary-tract-infections
- https://www.urologyhealth.org/urology-a-z/u/urinary-tract-infections-in-adults
- https://www.nhsinform.scot/illnesses-and-conditions/kidneys-bladder-and-prostate/urinary-tract-infection-uti
- https://www.niddk.nih.gov/health-information/urologic-diseases/bladder-infection-uti-in-adults
- https://www.webmd.com/women/your-guide-urinary-tract-infections
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/urinary-tract-infections-uti
- https://www.nhs.uk/conditions/urinary-tract-infections-utis/
- https://www.healthline.com/health/urinary-tract-infection-adults