Latex agglutination test is a simple serological test where antigen and antibody reaction is made visible on the surface of latex particles. It is the process in which latex beads are coated either with antigen or with antibody and when a sample containing the corresponding component is added, the beads is clumped together forming visible agglutination. It is a rapid method used for the detection of antigen or antibody in different clinical samples.
This test is based on passive agglutination. In this reaction, the antigen or the antibody is attached with an inert carrier surface like latex so that the reaction becomes visible. It is the same basic principle in which particulate antigen reacts with its specific antibody in presence of electrolytes and suitable pH, and agglutination is produced. This is referred to as a particle agglutination test.
In this test, latex beads (polystyrene particles) are sensitized with known antigen or antibody. When the patient sample is mixed with these coated beads, the specific binding makes the particles cross-link. This reaction is seen as clumps on the slide. It is the positive indication that the sample contains the suspected substance. The reaction is completed within minutes and does not need any complicated equipment.
Latex agglutination test is used in diagnosis of many infectious diseases. Some of the main applications are detection of Cryptococcal antigen in CSF and detection of rheumatoid factor in serum. It is valued as it is rapid, inexpensive and the result is easy to interpret. It is also used in autoimmune disorders and for quick screening of different microbial antigens.
This test is useful but there are some limitations. False positive reaction may occur when there is non-specific aggregation of particles. Very high concentration of antigen may also cause false negative due to the prozone effect. Because of these, the result is often confirmed by other methods when necessary.
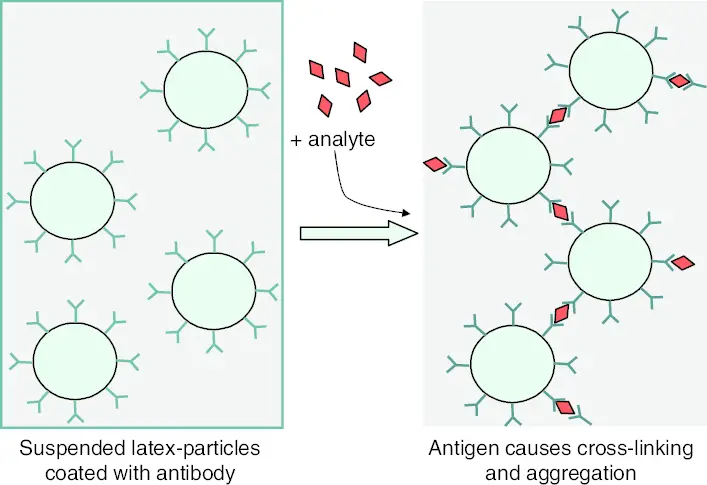
Types of Latex Agglutination
Latex agglutination can be divided into two main types depending on how the antigen and antibody is arranged on the latex surface. It is the process in which either antigen or antibody is coated on latex beads so that the reaction becomes visible by clumping. These types help in detecting antibody or antigen in the patient sample.
1. Latex Agglutination Test for Antibody Detection
In this type, the antigen is coated on the latex surface. It is the passive agglutination method where the sample containing antibodies is mixed with these sensitized beads. If the specific antibody is present, it binds with the antigen and the particles is agglutinated. It is useful to detect previous or current immune response as the presence of antibody shows exposure to that antigen. The clumping of beads is taken as the positive result.
2. Latex Agglutination Test for Antigen Detection
This is referred to as reverse passive agglutination test. Here the antibody is coated on the latex beads. When the patient sample containing antigen is added, the antigen binds with the antibody present on the beads. The reaction is seen as visible clumping. It is used to detect the presence of antigen in ongoing infection. It is the process that can show the presence of microbial antigen or foreign substance in the sample.
Both of these types are simple and rapid. The reaction is finished in a short time and only a small quantity of sample is needed. These tests are used widely in clinical laboratories as they have good sensitivity for detecting many antigen and antibody in patient samples.
Principle of Latex Agglutination
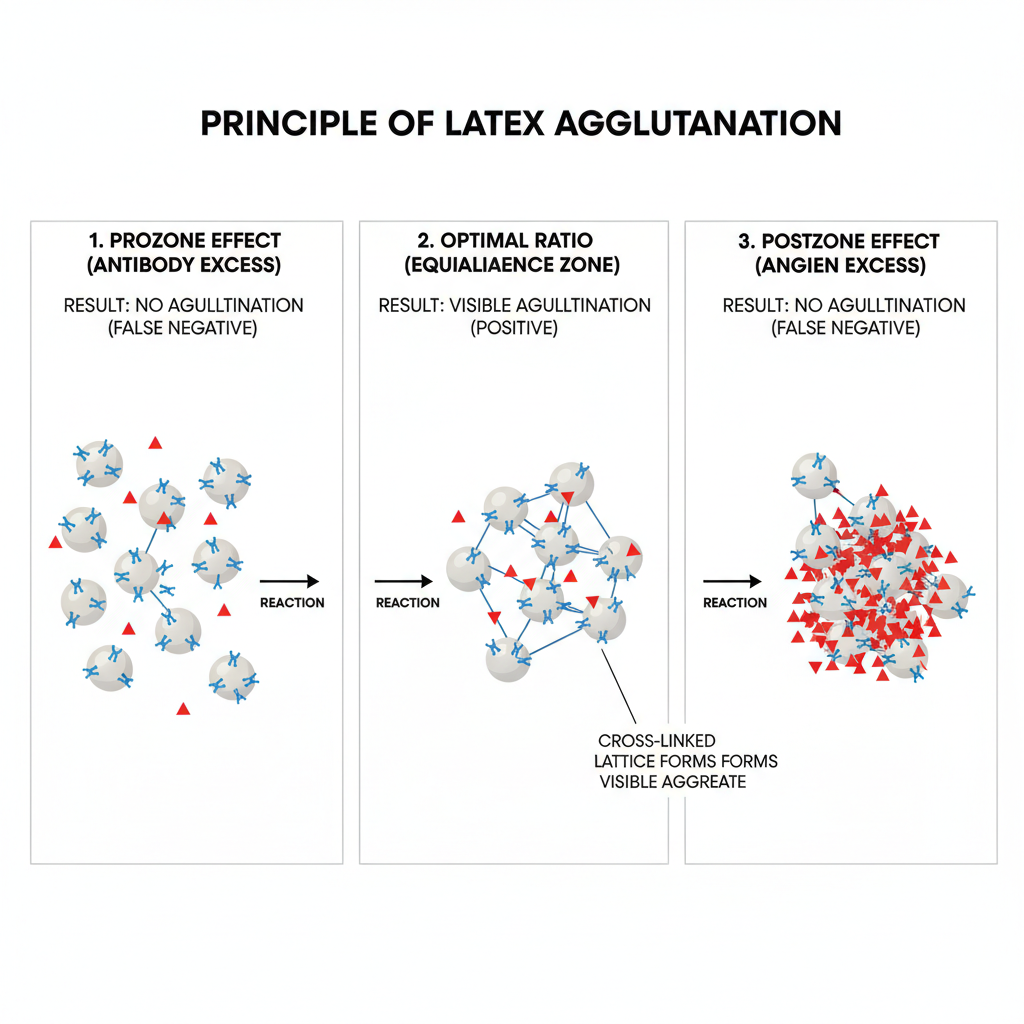
Latex agglutination is based on the passive agglutination principle in which latex beads act as the carrier surface for antigen or antibody. It is the process where a large number of antigen or antibody molecules is randomly attached on polystyrene particles so that many combining sites remain exposed on the bead surface. When the patient sample containing the corresponding antigen or antibody is added, the specific binding occurs on these exposed sites and the beads is cross-linked into visible aggregates. The reaction is easily seen because the particle size of latex is large and the clumping becomes clearly visible on the slide.
It is the principle that depends on formation of a lattice between the sensitized beads and the analyte present in the sample. When the ratio of antigen and antibody falls in an optimum range, the cross-linking forms a three-dimensional network which is taken as the positive reaction. It is affected when the concentration is very high either for antigen or antibody, as the prozone or postzone effect may inhibit proper lattice formation and the clumping is not produced. This is referred to as false negative reaction. The test is therefore considered a rapid serological method that detects antigen or antibody by the visible agglutination produced due to the reaction occurring on the latex surface.
Objectives of Latex Agglutination Test
The main objective of latex agglutination test is to detect the presence of a specific antigen or antibody in the patient sample by a simple visible reaction. It is the process in which latex beads coated with known antigen or antibody is used so that the reaction becomes rapid and easy to interpret. The test aims to identify the suspected analyte in serum, CSF, urine or other clinical samples.
It is used to provide quick diagnostic information by showing agglutination within a short period. Another objective is to support early detection of infectious agents or immune factors without the need of complicated instruments. It also helps in screening large number of samples as the method is inexpensive and can be performed easily in routine laboratories.
Materials Required for Latex Agglutination Test
- 1.5 ml vials
- Microcentrifuge
- Pipette
- Microtips
- Laboratory refrigerator
- Glycine saline buffer
- Blocking buffer
- Antigen for coating
- Latex beads
- Test antiserum
- Glass slides
- Beaker
- Tooth pick
Procedure of Latex Agglutination Test
Common to both types of latex tests is the encapsulation of latex microbeads with pathogen-specific antigens or antibodies. The cerebrospinal fluid, serum, or urine of the patient is mixed with coated latex particles in serial dilutions of normal saline, and agglutination (clumping) is observed.
A. Coating of Latex
Coating the latex beads for the detection of antibodies involves several steps. The following are the steps involved in the coating process:
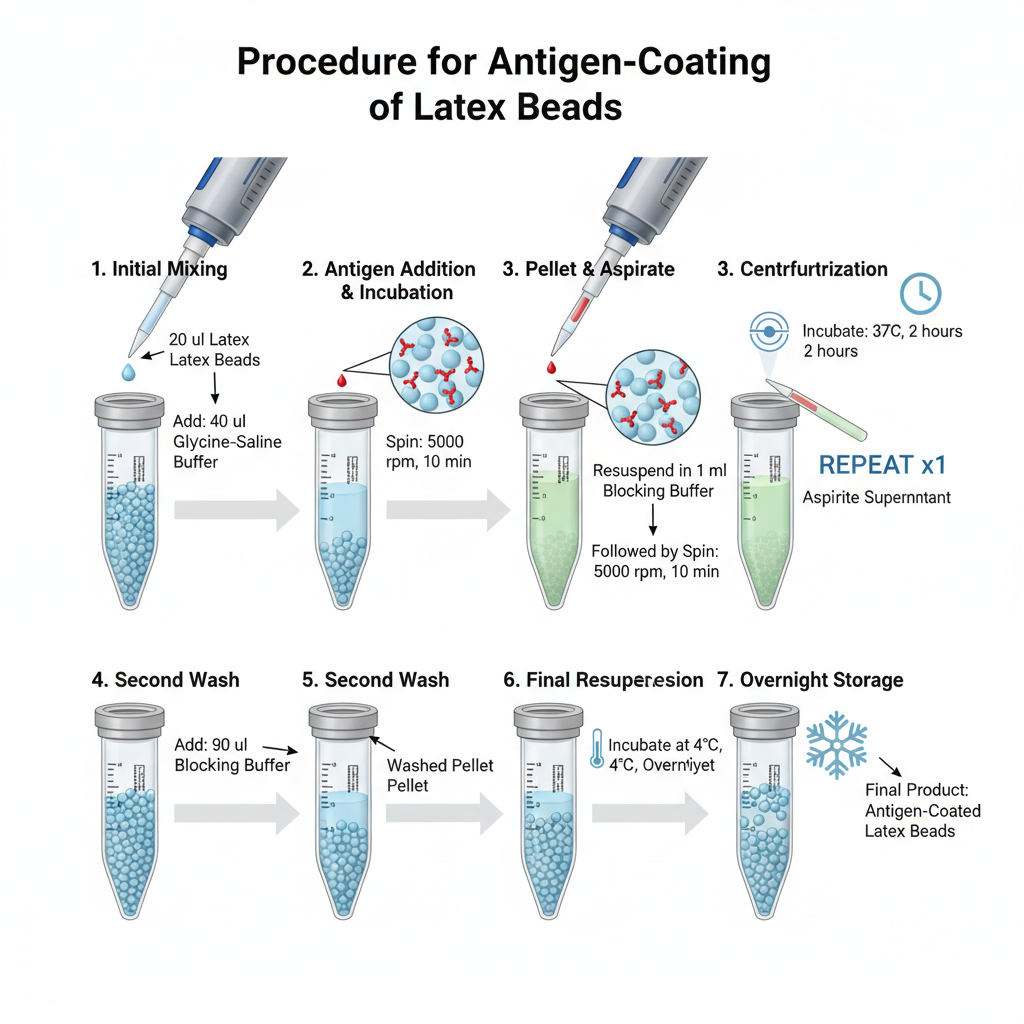
- Take 20 µl of latex beads in a 1.5 ml vial. These beads act as the carrier particles for the antigen.
- Add 40 µl glycine-saline buffer to the vial. It is used to wash and dilute the beads.
- Add 60 µl of the specific antigen and mix properly. It is the step where antigen is allowed to contact the bead surface.
- Incubate the vial at 37°C for 2 hours. It is the process where antigen is attached to the latex beads.
- Centrifuge at 5000 rpm for 10 minutes. The pellet formed is the coated bead-antigen complex.
- Remove the supernatant carefully without disturbing the pellet.
- Resuspend the pellet in 1 ml blocking buffer. This buffer is used to reduce non-specific binding.
- Centrifuge again at 5000 rpm for 10 minutes to wash away unbound antigen.
- Repeat the washing step one more time for proper removal of remaining antigen.
- Add 90 µl blocking buffer to the pellet and mix well so the coated beads are suspended evenly.
- Incubate the vial overnight at 4°C. This step is referred to as stabilization of coated latex beads for further use.
B. Agglutination Test
The agglutination test involves several steps to observe and interpret the results. Here are the steps to perform the agglutination test:
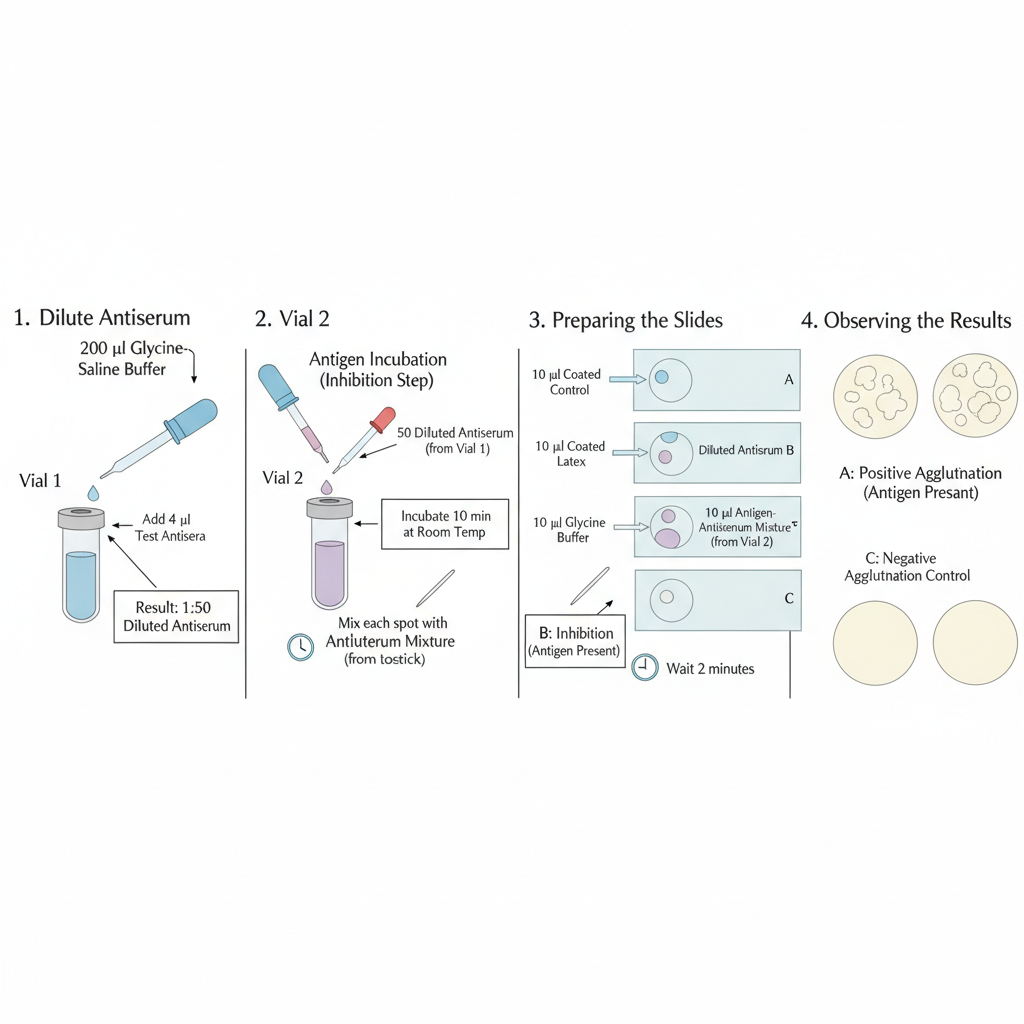
- Take 200 µl glycine-saline buffer in a vial. It is the buffer that makes a suitable condition for the agglutination reaction.
- Add 4 µl of test antisera (50× diluted) to the buffer. This antisera contain the antibodies for the reaction.
- In another 1.5 ml vial, mix 50 µl antigen with 50 µl diluted antisera. It is mixed properly and incubated at room temperature for 10 minutes.
- Pipette 10 µl coated latex on a clean glass slide. This latex is already coated with the required antigen.
- Add 10 µl diluted test antiserum to slide A. This is the antiserum that will react with the coated latex.
- Add 10 µl of the antigen–antisera mixture to slide B. It is used to show the antigen–antibody reaction.
- Add 10 µl glycine-saline buffer to slide C. It is the negative control slide.
- Mix each slide with a separate toothpick so there is no contamination.
- Allow the slides to stand for 2 minutes and observe the formation of agglutination.
Results and Interpretation of Latex Agglutination Test

Qualitative Interpretation
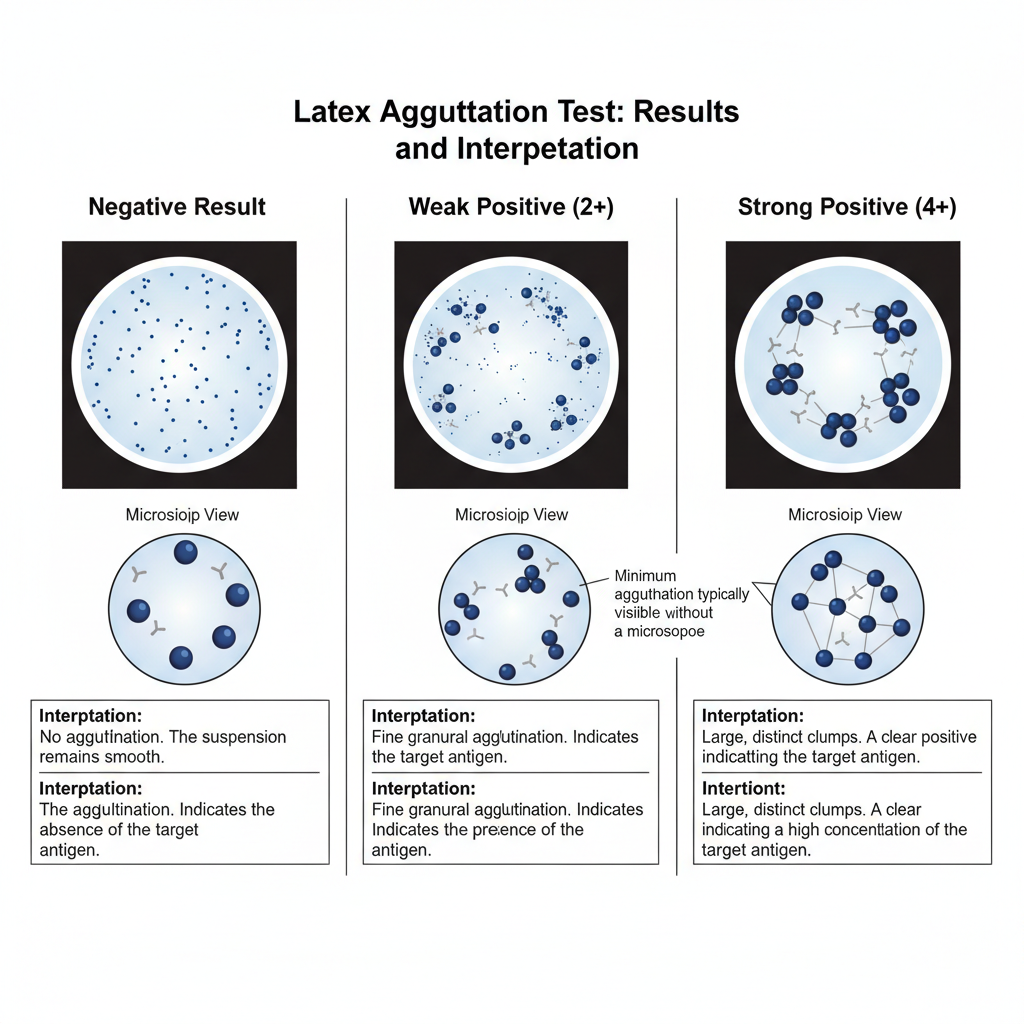
- A positive reaction is seen when clear clumping of latex particles is formed. It is the indication that the antigen or the antibody is present in the sample and the immune complex is formed.
- In some tests like Rheumatoid Factor detection, the agglutination is taken as the presence of RF in detectable amount.
- A negative reaction shows a uniform milky suspension without any clumps. It means the detectable analyte is absent under the test condition.
- In some antigen tests the titer below the required level is taken as not detected. It is important that a negative result can be true negative or may be due to improper test condition.
Semi-Quantitative Interpretation
- The test can be used for titration by making serial dilutions of the sample.
- It is the process where each dilution is checked for visible agglutination.
- The titer is the highest dilution that still gives a clear agglutination reaction.
- Increasing titers are taken as sign of progressive infection, and decreasing titers is taken as improvement.
- The reaction can be graded as 1+ to 4+ where 2+ is generally taken as minimum visible reaction.
Critical Issues and False Results
- In some cases false-negative reaction is seen due to excess antibody which is referred to as prozone effect. It is the condition where excess antibody saturate the antigenic sites and no lattice is formed. Dilution of the sample helps in avoiding this effect.
- False-negative reaction can also occur when excess antigen is present which is referred to as postzone effect. Here excess antigen occupy the antibody sites and prevent cross linking.
- False-positive reaction may occur when rheumatoid factor bind non-specifically with IgG coated latex. Pre-treatment of the sample is used to remove such interfering proteins.
- Antigen masking due to high protein or antigen-antibody complexes can also give false-negative reaction. Specific digestion methods help in unmasking the antigen.
- Very low titer of antibody may not give visible agglutination and can be seen as negative.
Applications of Latex Agglutination Test
- It is used in infectious disease diagnosis because latex beads can be coated with antigen or antibody for rapid detection.
- It is applied for detecting cryptococcal antigen in CSF and serum. It gives titers that help in following the disease condition and improvement after therapy.
- It is used for quick identification of bacteria like Staphylococcus aureus by detecting Protein A or clumping factor.
- It is used for grouping of Streptococcus species by detecting the Lancefield antigens.
- It is used for detecting capsular antigens of Haemophilus influenzae and Neisseria meningitidis in body fluids.
- It can detect E. coli serogroups and toxins in clinical and veterinary samples.
- It is useful in detecting antibodies in melioidosis and toxins of Clostridium difficile.
- It can be applied in detecting antiplague antibodies by using coated latex particles.
- It is used for viral and parasitic conditions like HIV, infectious mononucleosis, rubella, syphilis, HSV and Toxoplasma gondii.
- It is used for screening in visceral leishmaniasis though cross reaction can occur.
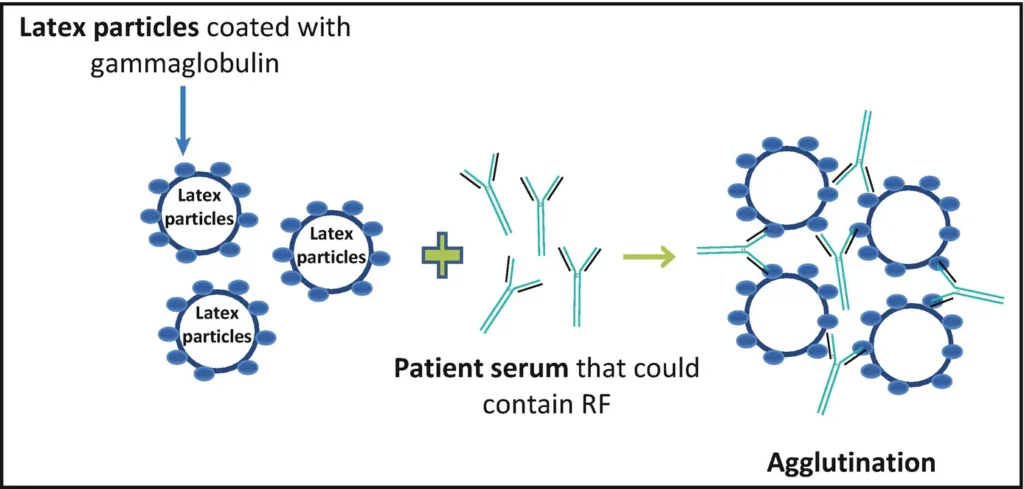
- It is useful in autoimmune disorders for detecting rheumatoid factor where IgG coated beads react with RF.
- It is applied for detecting C-reactive protein using latex coated with anti-CRP antibody.
- It is used for detecting antistreptolysin O antibodies in serum.
- It is useful in hematology for detecting von Willebrand factor antigen in plasma samples.
- It is used in agglutination inhibition tests for small antigens like hormones. For example, HCG detection in pregnancy kits.
- It is used as a general screening test in serum, CSF, urine and saliva due to its rapid reaction time.
Latex agglutination inhibition test
It is a modified form of latex agglutination where the reaction is used for detecting small soluble antigen present in the sample. It is the process in which the absence of clumping becomes the indicator for antigen because the antigen inhibits the agglutination reaction.
Principle
It is based on the inhibition of agglutination. In a normal latex agglutination reaction the antibody reacts with antigen-coated latex particles and visible clumping is formed. In this test the soluble antigen present in the patient sample binds with a limited amount of specific antibody and prevents the antibodies from reacting with the coated latex particles. This is referred to as agglutination inhibition.
Components
Some of the main components are–
- Latex particles coated with known antigen (e.g. HCG).
- A limited amount of specific antibody for that antigen.
Mechanism
The reaction is as follows–
In the first step the sample suspected to contain soluble antigen is mixed with a fixed small quantity of antibody. If antigen is present it binds to these antibodies. The sensitized latex particles are then added. Because the antibodies are already occupied by soluble antigen, no free antibody is present to cross-link the coated latex particles and the agglutination is inhibited. When the antigen is absent the antibodies remain free and agglutination is formed.
Interpretation
The absence of visible clumping indicates the presence of soluble antigen in the sample. It is the positive test. These are sensitive reactions used for detecting hormones and other low-molecular-weight antigens.
Example
Among the important applications is the detection of HCG hormone in pregnancy testing. It is the process where HCG in urine saturates the antibody and the HCG-coated latex particles do not agglutinate, showing a positive result.
Uses
Some of the uses are–
- Detection of hormones like HCG.
- Detection of small molecular antigens present in very low concentration.
Advantages of Latex Agglutination Test
- It is a rapid test where results are obtained within a short time, often within minutes, so it is suitable in urgent clinical conditions.
- The procedure is simple to perform and interpret. It does not require complex instruments and the reaction is seen directly by eye.
- It is cost-effective which makes it useful for routine screening work.
- It can be used in places with limited facilities because no specialized equipment is needed.
- The reaction is easily visible because latex beads form clear clumps that can be seen without magnification.
- It can give semi-quantitative information when serial dilution is done, which helps in following the progress of disease conditions.
- The method is versatile as coated latex can be used to detect either antibody or antigen depending on the test design.
- The reagents show good stability and can detect low amount of antigen in some tests.
Limitations of Latex Agglutination Test
- The test can give false-negative reaction when excess antibody is present. This is referred to as prozone effect where no visible lattice is formed.
- False-negative reaction can also occur in antigen excess condition which is referred to as postzone effect.
- False-positive reaction is seen when interfering substances like rheumatoid factor bind non-specifically to IgG coated latex.
- Cross reaction with non-target organisms may occur and reduce the specificity of the test.
- Non-specific clumping or contamination can also produce false-positive reaction.
- The reaction is sensitive to pH, ionic strength and other conditions, so strict standardization is needed.
- Some samples need pre-treatment like heating or chemical digestion which increases the steps of the procedure.
- Interpretation is done visually so it is subjective and depends on the user.
- The sensitivity is lower compared to advanced methods like ELISA.
- The coating of latex beads by passive adsorption may have limited stability and can be displaced by other molecules in the sample.
- Semi-quantitative results may vary because threshold values are not fully standardized.
FAQ
What is a latex agglutination test?
It is a diagnostic test where latex beads coated with antigen or antibody is mixed with the sample. The reaction is the formation of visible clumping when the corresponding antibody or antigen is present.
What is the principle of the latex agglutination test?
It is the process of antigen-antibody interaction. The coated latex beads react with the complementary antigen or antibody and the reaction is referred to as agglutination.
What is the purpose of the latex agglutination test?
The major purpose is to detect soluble antigen or antibody in different clinical samples. It is used for quick identification of microorganisms and immune factors.
How is a latex agglutination test performed?
- A drop of sample is placed on a slide.
- Latex reagent is added and mixed properly.
- The mixture is rotated gently and observed.
- Visible clumping is the indication of a positive reaction.
What diseases can be diagnosed using the latex agglutination test?
These are used in detecting bacterial meningitis, rheumatoid arthritis, rotavirus, Cryptococcus antigen, Staphylococcus aureus, and other infections depending on the reagent.
What are the different types of latex agglutination tests?
Some of the types are–
– Direct latex agglutination
– Indirect or passive agglutination
– Reverse passive agglutination
What are the advantages of the latex agglutination test?
It is rapid and simple.
Small sample volume is required.
The process is done without complex equipment.
What are the limitations of the latex agglutination test?
False positive reactions can occur.
The process is affected by interfering substances.
Sensitivity is lower compared to other immunoassays.
What is a positive result in a latex agglutination test?
A positive result is the appearance of visible clumping on the slide. It is the indication that the specific antigen or antibody is present in the sample.
What is the role of latex beads in an agglutination test?
These beads provide a large surface for adsorption of antigen or antibody. They make the clumping reaction easily visible due to bead aggregation.
What is the difference between direct and indirect agglutination?
In direct agglutination, natural antigens react directly with antibody-coated latex beads.
In indirect agglutination, antigen is artificially attached to latex beads and reacts with antibody in the sample.
What is reverse passive agglutination?
It is the method where antibody is coated on latex beads and the antigen in the sample reacts with these coated beads to produce agglutination.
What samples are used for latex agglutination tests?
The common samples are serum, plasma, CSF, urine, and other body fluids depending on the antigen required.
What is the difference between latex agglutination and ELISA?
Latex test is based on visible clumping while ELISA is based on enzyme-substrate color reaction.
Latex test is mostly qualitative.
ELISA is more sensitive and can be quantitative.
What is the BactiStaph Latex Agglutination Test used for?
It is the process used for rapid identification of Staphylococcus aureus. The reaction is due to clumping factor and protein-A present on S. aureus which reacts strongly with the latex reagent.
- Smits HL, van der Hoorn MA, Goris MG, Gussenhoven GC, Yersin C, Sasaki DM, Terpstra WJ, Hartskeerl RA. Simple latex agglutination assay for rapid serodiagnosis of human leptospirosis. J Clin Microbiol. 2000 Mar;38(3):1272-5. doi: 10.1128/JCM.38.3.1272-1275.2000. PMID: 10699040; PMCID: PMC88605.
- https://www.clinisciences.com/en/read/serological-tests-in-mycology-1190/latex-agglutination-assays-2091.html
- https://vlab.amrita.edu/?sub=3&brch=69&sim=195&cnt=1
- https://miravistalabs.com/medical-fungal-infection-testing/antigen-detection/cryptococcus-latex-agglutination-test/
- https://www.lornelabs.com/news-events/blog/everything-you-should-know-about-latex-agglutination-tests
- https://www.ucsfhealth.org/medical-tests/003334
- https://microbeonline.com/immunology-note/
- https://vlab.amrita.edu/?sub=3&brch=69&sim=195&cnt=2
- https://www.ucsfbenioffchildrens.org/tests/003334.html
- https://www.lornelabs.com/news-events/blog/everything-you-should-know-about-latex-agglutination-tests
- https://medlineplus.gov/ency/article/003334.htm
- https://microbenotes.com/latex-agglutination-test/#applications-of-latex-agglutination-test