What is Urinary Tract Infection (UTI)?
Urinary Tract Infection (UTI) is a common bacterial infection of urinary system. It is affecting any part of the urinary system which includes bladder, urethra, ureters and kidneys. It is most frequently caused by Escherichia coli (E. coli). It occurs more often in women than in men.
UTI is mainly categorized into two types. Uncomplicated UTI is a simple infection usually confined to bladder in otherwise healthy individuals. This is also referred to as cystitis. Complicated UTI is a more severe infection where kidneys can be involved or it occurs in males, pregnant women, individuals with catheter or persons with underlying health conditions.
The symptoms includes burning sensation or pain during urination (dysuria). Sudden and frequent urge to urinate cloudy urine or blood tinged urine and lower abdominal or pelvic discomfort are also seen. It is treated by antibiotics in most cases but it is important to treat it promptly. If it is not treated infection can spread to kidneys and more serious complications are caused.
Types of Urinary Tract Infection (UTI)
Types of Urinary Tract Infection (UTI) are classified in different ways. These are as follows–
- By Anatomical Site (Location)
- Lower urinary tract infection (lUTI) – It includes cystitis(infection of bladder) and urethritis(infection of urethra).
- Upper urinary tract infection (uUTI) – It includes pyelonephritis(infection of kidneys) and urosepsis.
- By Clinical Complexity
- Uncomplicated( simple) UTI – It is infection occurs in otherwise healthy individuals without structural or neurological urinary tract abnormality.
- Complicated UTI – It occurs in individuals with risk factors like anatomical abnormality urinary stones catheter immunosuppression or pregnancy.
- By 2025 European Association of Urology (EAU) classification
- Localized UTI – It is cystitis presenting without any signs or symptoms of systemic infection.
- Systemic UTI – It is UTI with systemic signs and symptoms like fever chills or hypotension indicating infection may spread beyond bladder.
- By Frequency and Chronicity
- Recurrent UTI – It is two or more acute UTIs within 6 month period or at least three within 12 month period.
- Relapsing UTI – It is recurrence of original infection by same bacterial strain usually within two weeks after completing antibiotic treatment.
- Re-infection – It is a new infection caused by different bacterial organism usually diagnosed more than two weeks after previous treatment.
- Persistent UTI – It is ongoing presence of same pathogen in urine culture despite treatment.
- Other specific types and presentations
- Catheter-associated UTI (CAUTI) – It occurs in patients with indwelling urinary catheter and it represent a large portion of complicated UTI.
- Asymptomatic bacteriuria – It is presence of bacteria in urine without any clinical signs or symptoms of infection.
- Urosepsis – It is severe life threatening systemic infection and organ dysfunction originating from UTI.
Causative Agents of UTI
Causative agents of UTI are mainly bacteria. These are as follows–
- Gram-negative bacteria
- Escherichia coli (Uropathogenic E. coli or UPEC) – It is most common causative agent in uncomplicated and complicated UTI.
- Klebsiella species – K. pneumoniae, K. oxytoca.
- Proteus species – P. mirabilis, P. vulgaris.
- Pseudomonas species – P. aeruginosa.
- Enterobacter species – E. cloacae, E. aerogenes.
- Citrobacter species – C. freundii.
- Acinetobacter species – A. baumannii, A. lwoffii.
- Morganella morganii.
- Serratia species – S. marcescens.
- Pantoea agglomerans.
- Acetobacter species.
- Gram-positive bacteria
- Staphylococcus species – Staphylococcus saprophyticus, Staphylococcus aureus(including methicillin-resistant S. aureus or MRSA), Staphylococcus haemolyticus and other coagulase-negative staphylococci.
- Enterococcus species – E. faecalis.
- Group B Streptococcus (GBS).
- Lactobacillus species.
- Other bacteria
- Ureaplasma urealyticum.
- Fungi/yeasts
- Candida species – C. albicans, C. tropicalis, C. glabrata
Risk factors of UTI
Risk factors of UTI are conditions which increases the chance of infection. These are as follows–
- Demographic and biological factors
- Female sex – It is more common in women due to shorter urethra which allows bacteria to ascend easily.
- Age extremes – It is seen more in geriatric patients and infants.
- Menopause – It leads to atrophic vaginitis and decrease in protective vaginal flora.
- Genetic predisposition – It is seen in individuals having mother or sister with history of frequent UTI.
- Sexual and behavioral factors
- Frequent sexual intercourse or new/multiple sexual partners.
- Use of diaphragm spermicides or spermicide coated condoms.
- First UTI before age of 16 years.
- Inadequate fluid intake or dehydration.
- Anatomical and functional abnormalities
- Urinary tract obstruction – Kidney stones bladder stones and prostate enlargement in men.
- Incomplete bladder emptying or high post void residual urine volume.
- Pelvic organ prolapse – Cystocele(dropped bladder).
- Vesicoureteral reflux – It is backward flow of urine from bladder to kidneys.
- Functional defects – Neurogenic bladder overactive bladder and urinary incontinence.
- Structural defects – Urethral or bladder diverticula and fistulas.
- Medical conditions and immunity
- Diabetes and obesity.
- Immunocompromised states – HIV chemotherapy or steroid use.
- Renal failure dialysis or history of kidney transplantation.
- Spinal cord injuries and chronic diarrhea.
- Healthcare interventions
- Indwelling urinary catheter or suprapubic tube.
- Recent urological instrumentation surgeries or frequent pelvic examination.
- Prior antibiotic use – It alters normal flora and resistant organisms are developed.
- Use of certain diabetes drugs causing glucose in urine(SGLT2 inhibitors like dapagliflozin).
- Personal hygiene practices
- Wiping from back to front after toilet use.
- Taking bath instead of shower and using reusable luffas or sponges.
- Not washing hands before wiping or improper cleaning of genital area.
Symptoms of UTI
Symptoms of UTI are the clinical features seen during infection. These are as follows–
- Pain burning or stinging sensation during urination(dysuria).
- Sudden strong and frequent urge to urinate.
- Difficulty in starting urine stream(hesitancy).
- Cloudy dark bad smelling or blood tinged urine(hematuria).
- Pressure cramping or pain in lower abdomen(suprapubic pain).
- Bladder spasms.
- New or worsening urinary incontinence.
- Pus discharge from urethra(urethral purulence).
If infection spreads beyond bladder and becomes systemic the following symptoms are seen–
- Fever or abnormally low body temperature(hypothermia).
- Shaking chills or rigors.
- Flank back or costovertebral angle pain.
- Nausea and vomiting.
In older adults or frail patients atypical symptoms are seen. These are–
- Confusion delirium or sudden change in mental status.
- Unexplained weakness severe fatigue or lethargy.
Pathogenesis of UTI
Pathogenesis of UTI is the sequence of events by which infection is developed in urinary tract. It is mainly caused by Uropathogenic Escherichia coli(UPEC). The process is as follows–
- It begins with contamination and colonization of periurethral area by bacteria from gastrointestinal tract(rectal and perineal flora).
- The bacteria ascends through urethra and reaches urinary bladder. This movement is facilitated by flagella which helps in moving against the flow of urine.
- In bladder the bacteria attaches to umbrella cells by pili or fimbriae(Type 1 pili). It is tightly bound to bladder wall and washing out during urination is prevented.
- The bacteria invades bladder epithelial cells and enters into cytoplasm. It multiplies rapidly and Intracellular Bacterial Communities(IBCs) is formed. It is protected from immune response and antibiotic action in this stage.
- The host immune system sends neutrophils to bladder. The infected superficial cells undergo exfoliation and bacteria are expelled into urine.
- Some bacteria changes into filamentous form and resists phagocytosis. Biofilm is also formed on bladder tissue or on urinary catheter.
- After shedding of superficial cells bacteria invades deeper layers and enters dormant stage called Quiescent Intracellular Reservoirs(QIRs). These bacteria persists for long time and recurrent UTI is caused.
- If infection is not cleared bacteria ascends through ureters to kidneys. It uses P pili to attach renal tissue and pyelonephritis is developed.
- In kidney toxins like hemolysin and proteases are secreted and host tissue is destroyed. If untreated bacteria enters bloodstream and bacteremia or urosepsis is produced.
Diagnosis of UTI
Diagnosis of UTI is based on clinical features and laboratory investigations. The methods are as follows–
- Clinical history and physical evaluation – It is the initial step in diagnosis. The history of dysuria frequent urge to urinate cloudy urine and lower abdominal or pelvic pain is taken. Physical examination is also done to assess tenderness or discomfort.
- Proper urine specimen collection – An uncontaminated urine sample is required for accurate testing. Midstream clean catch specimen is collected in adults and toilet trained children. In infants below 3 months or in patients unable to give clean sample catheterized specimen is recommended.
- Rapid urinalysis(Urine dipstick test) – It is a quick screening test done in clinic to detect markers of infection.
- Nitrites – It detects bacteria like E. coli which reduces nitrate to nitrite. It is highly specific for UTI.
- Leukocyte esterase(LE) – It detects enzyme released by white blood cells and indicates pyuria or inflammation.
- Blood – It detects hematuria which occurs due to infection of bladder lining.
- Microscopic urine analysis – Urine is examined under microscope. Presence of white blood cells(red blood cells) and bacteria are confirmed. Pyuria is commonly seen.
- Urine culture and sensitivity testing – It is considered as gold standard for diagnosis of UTI.
- Culture – It identifies exact bacterial strain and measures bacterial count. A count of ≥10⁵ colony forming units(CFU)/mL is significant but in symptomatic women lower counts like ≥10²–10⁴ CFU/mL is also diagnostic.
- Sensitivity – It determines which antibiotics the bacteria is susceptible or resistant and helps in selecting proper treatment.
- Urological imaging(Ultrasound or CT scan) – It is not routinely required in simple UTI. It is recommended if patient does not respond to antibiotics within 48–72 hours to rule out stones obstruction or abscess. Renal ultrasound is also advised in children below 2 years with first febrile UTI.
- Cystoscopy – It is direct visualization of inside of bladder using scope. It is done in relapsing or recurrent infections or when anatomical abnormality foreign body or unexplained gross hematuria is suspected.
Treatment of UTI
Treatment of UTI is based on type and severity of infection. It includes antimicrobial therapy symptomatic relief and preventive measures. These are as follows–
- Treatment of uncomplicated(simple) UTI
- Nitrofurantoin – It is used as first line therapy for 5–7 days.
- Sulfamethoxazole-trimethoprim(SMX-TMP) – It is commonly given for 3 days if local resistance is low.
- Fosfomycin – It is administered as single oral dose.
- Pivmecillinam – It is extended spectrum penicillin approved for first line oral therapy.
- Alternative oral antibiotics – Beta lactams like amoxicillin-clavulanate or cephalosporins and fluoroquinolones like ciprofloxacin or levofloxacin is used when first line drugs cannot be prescribed or fail.
- Treatment of complicated UTI
- Intravenous(IV) antibiotics – Severe cases or sepsis requires broad spectrum IV antibiotics such as third or fourth generation cephalosporins(ceftriaxone cefepime) carbapenems or piperacillin-tazobactam.
- Advanced antibiotics for resistant strains – Newer drugs like ceftazidime-avibactam or cefiderocol is used in multi drug resistant(MDR) infections.
- IV to oral transition – When patient shows clinical improvement IV antibiotics is changed to oral therapy to complete course.
- Shorter treatment course – Current guidelines recommends 5–7 days of fluoroquinolones or 7 days of non fluoroquinolones in patients with good clinical response.
- Symptomatic relief
- Urinary analgesics – Phenazopyridine(AZO or Pyridium) relieves burning and pain but it should not be used more than 48 hours.
- General pain relievers – NSAIDs like ibuprofen or acetaminophen reduces pain and bladder spasms.
- Prevention and management of recurrent UTI
- Antibiotic prophylaxis – Continuous low dose daily antibiotic or single dose post coital antibiotic is given.
- Self start therapy – Patient is prescribed short course antibiotic to start at first sign of symptoms.
- Vaginal estrogen – Topical estrogen therapy is recommended in perimenopausal and postmenopausal women to maintain urethral tissue health.
- Non antibiotic supplements – Cranberry products D-mannose probiotics(Lactobacillus) and methenamine hippurate are used to reduce recurrence.
- Hydration and behavioral changes – Increased fluid intake(1.5–2 liters per day) and modification of hygiene or contraceptive practice is advised.
- Vaccines – Immunostimulants like MV140(Uromune) Uro-vaxom or Strovac helps in preventing recurrent UTI.
- Intravesical therapy – Bladder instillation with gentamicin hyaluronic acid or chondroitin is used in intractable cases.
Treatment of Urinary Tract Infections with D-Mannose
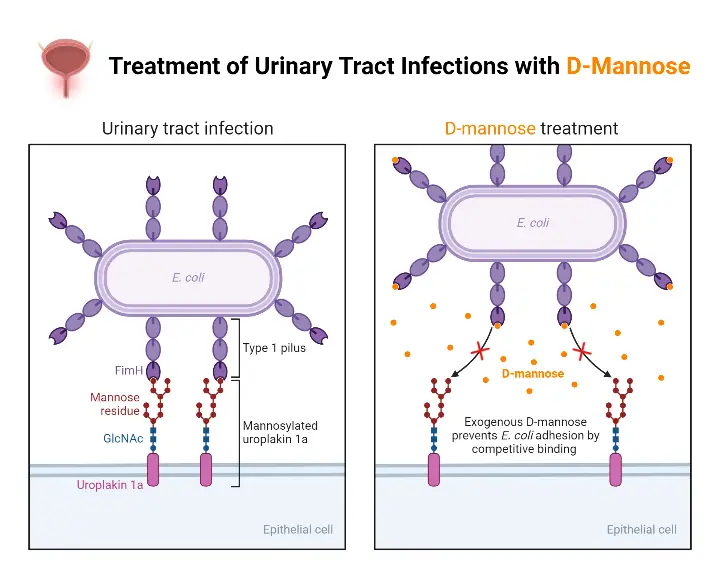
Treatment of Urinary Tract Infection with D-Mannose is used as non antibiotic therapy mainly for prevention of recurrent UTI. It acts by preventing bacterial adhesion to urinary tract epithelium. The details are as follows–
- Mechanism of action
- What it is – D-mannose is a simple sugar(monosaccharide) naturally present in diet and fruits like apples oranges and cranberries.
- How it works – It acts as molecular decoy by binding to surface ligand(FimH adhesin) of uropathogenic Escherichia coli(UPEC).
- Clearing of infection – After binding to bacteria it prevents adhesion and invasion of uroepithelial cells lining bladder wall. The bacteria is flushed out during urination.
- Dosage and administration
- Forms – It is available over the counter as oral tablets capsules and effervescent powders.
- Dose – In clinical studies dose ranges from 200 mg to 3 g per day. Common preventive dose is 2 g once daily. In early active symptoms 1.5 g three times daily is sometimes used.
- Combination therapy – It is frequently combined with cranberry extract vitamin C or probiotics to improve urinary tract health.
- Clinical efficacy and medical guidelines
- Conflicting evidence – Some earlier small studies showed reduction in recurrent UTI up to 45% and effect similar to prophylactic antibiotics.
- Lack of proven benefit – A 2022 Cochrane review reported very low certainty evidence and little reliable proof for treatment or prevention of UTI. Recent randomized trial showed no significant difference between 2 g D-mannose daily and placebo in recurrence rate.
- Current guidelines – 2025 American Urological Association(AUA) guidelines states insufficient evidence to recommend D-mannose alone for UTI prevention.
- Safety and side effects
- Safety profile – It is generally considered safe and serious harm is unlikely.
- Adverse effects – Mild gastrointestinal symptoms like diarrhea flatulence or vaginal burning may occur.
Animation Video
Prophylaxis and Prevention of UTI
Prophylaxis and prevention of UTI is important to reduce recurrence and complications. It includes behavioral measures non antibiotic methods and antibiotic prophylaxis. These are as follows–
- Behavioral and personal hygiene modifications
- Proper wiping – It should be done from front to back after urination or bowel movement to prevent transfer of bacteria from rectal area to urethra.
- Hand hygiene – Hands should be washed before toilet use and before wiping genital area.
- Bathing practices – Shower is preferred instead of bath and reusable luffas or sponges should be avoided.
- Washing technique – Clean gentle liquid soap without harsh perfume is used and urethral area is cleaned first with single use washcloth.
- Bladder emptying – Bladder should be emptied frequently(every 4 hours) and voiding after sexual intercourse is advised.
- Hydration – Daily fluid intake of 1.5–2 liters is recommended to maintain proper urine flow and flush out bacteria.
- Clothing and menstrual care – Tight clothing for prolonged period should be avoided and tampons may be preferred over sanitary pads.
- Contraceptive changes – Use of diaphragm and spermicide coated condoms should be avoided as it disrupts normal vaginal flora.
- Non antibiotic prophylaxis
- Cranberry supplements – Juice extract or tablets containing proanthocyanidins(PACs) inhibits adhesion of bacteria like E. coli to urothelium.
- D-mannose – It binds to bacterial surface ligand and prevents attachment to bladder wall.
- Topical vaginal estrogen – It is recommended in peri and postmenopausal women to restore Lactobacillus flora and maintain low vaginal pH.
- Probiotics – Lactobacillus strains are used orally or vaginally to restore microbial balance.
- Methenamine hippurate – It converts into bactericidal formaldehyde in acidic urine and sometimes vitamin C is given to acidify urine.
- Vaccines and immunotherapy – Bacterial vaccines like MV140(Uromune) Uro-vaxom or Strovac stimulates immune response against uropathogenic strains.
- Antibiotic prophylaxis(for recurrent cases)
- Continuous low dose prophylaxis – Low dose antibiotics like Nitrofurantoin Trimethoprim-sulfamethoxazole Trimethoprim or Fosfomycin is given daily for 6–12 months.
- Postcoital prophylaxis – Single dose antibiotic is taken before or after sexual intercourse when UTI is related to sexual activity.
- Self directed therapy – Short course antibiotic is provided to start at first sign of symptoms.
- Specialized clinical prevention strategies
- Intravesical therapy – Antimicrobial agents like gentamicin chlorhexidine or hyaluronic acid is instilled directly into bladder especially in neurogenic bladder or catheterized patients.
- Catheter management – Indwelling catheter should be avoided when possible removed early and sterile insertion technique is followed. Drainage bags should be changed regularly.
- Vesicoureteral reflux(VUR) management – Continuous antibiotic prophylaxis is used in children with VUR to prevent kidney infection and renal scarring.
FAQ
What is a urinary tract infection (UTI)?
A urinary tract infection is an infection that affects any part of the urinary system, including the kidneys, bladder, ureters, and urethra.
Can UTIs be prevented?
While UTIs cannot always be prevented, there are steps you can take to reduce the risk. These include staying hydrated, urinating after sexual activity, practicing good hygiene, avoiding irritating products in the genital area, and considering cranberry juice or supplements.
Who is at a higher risk of developing UTIs?
Women are more prone to UTIs due to their shorter urethra, which allows bacteria to reach the bladder more easily. Other risk factors include sexual activity, menopause, urinary tract abnormalities, catheter use, weakened immune system, and certain medical conditions.
How are UTIs diagnosed?
UTIs are typically diagnosed based on symptoms, a physical examination, and a urine sample analysis. Urinalysis and urine culture may be conducted to confirm the presence of bacteria and determine the specific type of bacteria causing the infection.
What is the treatment for a UTI?
The mainstay of UTI treatment is antibiotics prescribed by a healthcare professional. The specific antibiotic and duration of treatment depend on the type and severity of the infection. It is important to complete the full course of antibiotics as prescribed.
Can UTIs be recurrent?
Yes, UTIs can recur, especially in individuals with risk factors such as urinary tract abnormalities, frequent sexual activity, or a history of UTIs. Recurrent UTIs may require further evaluation and management by a healthcare professional.
Are there any complications associated with UTIs?
If left untreated or inadequately treated, UTIs can potentially lead to more serious complications, such as kidney infections (pyelonephritis), bloodstream infections (sepsis), and recurrent infections.
What are the common symptoms of a UTI?
Common symptoms of a UTI may include frequent urination, pain or burning sensation during urination, cloudy or bloody urine, strong-smelling urine, pelvic pain, and a feeling of urgency to urinate.
Can men get UTIs?
Although less common, men can also develop UTIs. In men, UTIs are often associated with underlying urinary tract abnormalities, such as an enlarged prostate or urinary stone.
When should I seek medical attention for a suspected UTI?
If you experience symptoms of a UTI, it is recommended to seek medical attention. Prompt diagnosis and treatment can help alleviate symptoms and prevent potential complications.
References
- Ackerman, A. L., Bradley, M., D’Anci, K. E., Hickling, D., Kim, S. K., & Kirkby, E. (2025). Updates to recurrent uncomplicated urinary tract infections in women: AUA/CUA/SUFU guideline. Journal of Urology. https://doi.org/10.1097/JU.0000000000004723
- Aggarwal, N., & Leslie, S. W. (2025). Recurrent urinary tract infections. In StatPearls. StatPearls Publishing.
- Ahmed, S. S., Shariq, A., Alsalloom, A. A., Babikir, I. H., & Alhomoud, B. N. (2019). Uropathogens and their antimicrobial resistance patterns: Relationship with urinary tract infections. International Journal of Health Sciences, 13(2), 48–55.
- Bonkat, G., Wagenlehner, F., Cai, T., Geerlings, S., Medina-Polo, J., Köves, B., … & Kranz, J. (2025). Classification of urinary tract infections in 2025: Moving beyond uncomplicated and complicated. European Urology Open Science, 75, 44–47. https://doi.org/10.1016/j.euros.2025.03.010.
- Bono, M. J., & Leslie, S. W. (2025). Uncomplicated urinary tract infections. In StatPearls. StatPearls Publishing.
- Flores-Mireles, A. L., Walker, J. N., Caparon, M., & Hultgren, S. J. (2015). Urinary tract infections: Epidemiology, mechanisms of infection and treatment options. Nature Reviews Microbiology, 13(5), 269–284. https://doi.org/10.1038/nrmicro3432.
- García-García, J. D., Contreras-Alvarado, L. M., Cruz-Córdova, A., Hernández-Castro, R., Flores-Encarnacion, M., Rivera-Gutiérrez, S., Arellano-Galindo, J., Ochoa, S. A., & Xicohtencatl-Cortes, J. (2025). Pathogenesis and immunomodulation of urinary tract infections caused by uropathogenic Escherichia coli. Microorganisms, 13(4), 745. https://doi.org/10.3390/microorganisms13040745.
- Hans, A., Yadav, A., Kaur, P., & Kumari, A. (2024). Evaluation of leukocyte esterase and nitrite dipstick tests with routine urine microscopic analysis in detecting urinary tract infections. Indian Journal of Pathology and Oncology, 11(1), 3–7. https://doi.org/10.18231/j.ijpo.2024.002.
- Sabih, A., & Leslie, S. W. (2024). Complicated urinary tract infections. In StatPearls. StatPearls Publishing.
- Semeniuk, H., & Church, D. (1999). Evaluation of the leukocyte esterase and nitrite urine dipstick screening tests for detection of bacteriuria in women with suspected uncomplicated urinary tract infections. Journal of Clinical Microbiology, 37(9), 3051–3052. https://doi.org/10.1128/jcm.37.9.3051-3052.1999.
- Terlizzi, M. E., Gribaudo, G., & Maffei, M. E. (2017). UroPathogenic Escherichia coli (UPEC) infections: Virulence factors, bladder responses, antibiotic, and non-antibiotic antimicrobial strategies. Frontiers in Microbiology, 8, 1566. https://doi.org/10.3389/fmicb.2017.01566.
- Trautner, B. W., Cortés-Penfield, N. W., Gupta, K., Hirsch, E. B., Horstman, M., Moran, G. J., … & Lavergne, V. (2025). Clinical practice guideline by Infectious Diseases Society of America (IDSA): 2025 guideline on management and treatment of complicated urinary tract infections: Executive summary. Infectious Diseases Society of America.
- Wiles, T. J., Kulesus, R. R., & Mulvey, M. A. (2008). Origins and virulence mechanisms of uropathogenic Escherichia coli. Experimental and Molecular Pathology, 85(1), 11–19. https://doi.org/10.1016/j.yexmp.2008.03.007.